What It Is
What Is Trigeminal
Neuralgia?
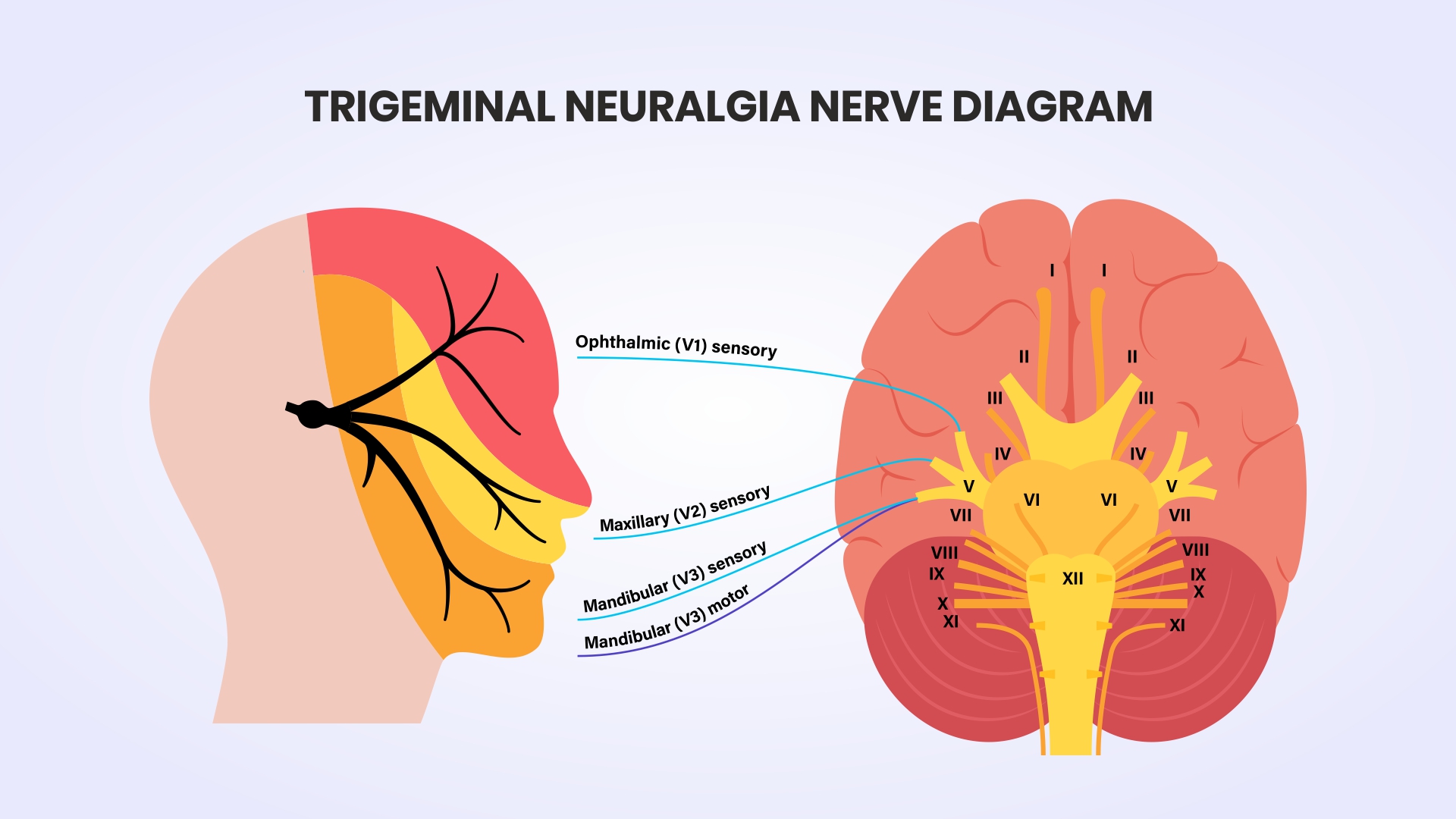
Trigeminal Neuralgia (TN) is a chronic pain condition affecting the trigeminal nerve — the fifth cranial nerve, and the largest of the cranial nerves. The trigeminal nerve carries sensation from the face to the brain, covering three divisions: the forehead and eye (V1), the cheek and upper jaw (V2), and the lower jaw and chin (V3).
TN causes sudden, severe, electric shock-like or stabbing facial pain that comes without warning and disappears as quickly as it arrived. The pain is typically on one side of the face and lasts from a fraction of a second to a few minutes. Between attacks, there may be no pain at all. However, attacks may occur many times a day and can be completely disabling.
Trigeminal Neuralgia is considered one of the most painful conditions known to medicine — it has been called the “suicide disease” because of the severity of untreated pain. However, with modern treatment — particularly MVD surgery — most patients can achieve long-term, durable pain relief.
Key Facts About Trigeminal Neuralgia
›Considered one of the most painful conditions known to medicine
›Electric shock-like pain lasting seconds to minutes per attack
›Triggered by eating, speaking, brushing teeth, or light touch
›Usually affects one side of face only
›MVD surgery: 80–90% long-term pain-free rate
›MRI essential before treatment to identify cause and plan surgery
Symptoms & Causes
Symptoms, Triggers
& Causes of TN
Characteristic Symptoms
✗Sudden severe pain: electric shock, stabbing, or shooting pain in the face — comes without warning
✗Duration: seconds to 2 minutes per episode; attacks may cluster many times per day
✗Location: cheek, jaw, teeth, gums, lips; V2 (upper jaw) and V3 (lower jaw) most commonly affected; V1 (eye, forehead) less common
✗Laterality: almost always unilateral (one side). Bilateral TN is rare and warrants investigation for MS.
✗Between attacks: pain-free periods between episodes; in later stages, a dull ache may persist
Common Triggers
›Eating or chewing
›Talking or smiling
›Brushing teeth
›Light touch on the face
›Wind or cold air
›Washing the face
›Applying makeup
›Swallowing
What Causes Trigeminal Neuralgia?
Primary Cause: Vascular Compression (Classical TN)
In the majority of TN patients, a blood vessel — usually the Superior Cerebellar Artery (SCA) or Anterior Inferior Cerebellar Artery (AICA) — presses against the trigeminal nerve root at its entry zone into the brainstem. This chronic pulsatile compression causes demyelination (damage to the protective sheath) of the nerve fibres, leading to abnormal electrical discharge and the characteristic pain.
Multiple Sclerosis (MS)
MS plaques can form at the trigeminal nucleus or nerve, causing TN. MS-related TN is more often bilateral. MRI identifies MS plaques and distinguishes MS-TN from classical vascular TN.
Tumour or Vascular Malformation
Occasionally a tumour at the cerebellopontine angle (acoustic neuroma, meningioma) or a vascular malformation compresses the trigeminal nerve. MRI identifies these secondary causes and guides treatment planning.
Treatment Options
Trigeminal Neuralgia
Treatment at KG Hospital
KG Hospital offers the complete range of Trigeminal Neuralgia treatments — from first-line medications through to definitive surgical cure. Treatment is selected based on patient age, general health, MRI findings, and preference.
01
Medication — First Line
Carbamazepine (Tegretol) or Oxcarbazepine are the first-line treatments. They reduce nerve firing and control pain in most patients initially. Over time, doses need to increase and side effects (drowsiness, dizziness, hyponatraemia) may become intolerable. When medications fail, surgical options are considered.
02
Microvascular Decompression (MVD)
Gold-standard surgery. Small posterior fossa craniotomy behind the ear. Offending vessel identified, repositioned, and a soft Teflon pad placed between vessel and nerve. 80–90% long-term pain-free rate. Facial sensation fully preserved. Best option for fit patients.
Gold Standard
03
Glycerol Rhizotomy
Percutaneous minimally invasive procedure. Thin needle guided under X-ray fluoroscopy through the cheek to the trigeminal cistern at the skull base. Glycerol injected to selectively damage pain-carrying fibres. Day procedure. ~80% initial pain relief. May need repetition as pain can recur.
04
Radiofrequency Thermal Lesioning
Percutaneous procedure under fluoroscopic guidance. A probe is advanced to the trigeminal ganglion and radio-frequency heat is applied to selectively destroy pain fibres. Provides 3–4 years of relief. Some facial numbness expected post-procedure. Day procedure.
Gold Standard Surgery
Microvascular Decompression (MVD)
The Definitive Treatment
Microvascular Decompression (MVD) is the most effective and durable treatment for Trigeminal Neuralgia and addresses the root cause directly: the blood vessel compressing the trigeminal nerve root. It is the only TN treatment that does not damage the nerve itself.
The procedure is performed under general anaesthesia through a small craniotomy behind the ear (posterior fossa approach). The neurosurgeon — using the TIVATO 700 surgical microscope for magnification and illumination — identifies the trigeminal nerve root at its entry into the brainstem. The offending blood vessel is gently separated from the nerve and a soft Teflon pad is placed between them to prevent re-contact. The craniotomy is then closed.
There is no destruction of any part of the trigeminal nerve. Facial sensation is fully preserved. Pain relief is typically immediate upon waking from anaesthesia in most patients.
MVD at KG Hospital — Key Facts
✓80–90% long-term pain-free rate — highest of any TN treatment
✓Facial sensation fully preserved — unlike ablative procedures
✓Pain relief immediate for most patients post-operatively
✓Addresses root cause — vessel decompressed, not nerve damaged
✓Performed under TIVATO 700 microscope for precision
✓Hospital stay 3–5 days; full recovery 2–4 weeks
✓MRI pre-operatively confirms compressing vessel and anatomy
When MVD is the Right Choice
MVD is preferred for: patients in good general health with classical TN (vascular compression confirmed on MRI), younger patients requiring long-term durable relief, patients who have failed medication, and patients for whom facial numbness (a consequence of ablative procedures) would be unacceptable.
Am I Suitable?
Who is a Candidate
for Each Treatment?
Treatment selection depends on general health, age, MRI findings, medication history, and the patient’s priorities. Below is a guide — your neurosurgeon will review your specific situation:
✓ Good MVD Candidates
Fit for general anaesthesia and posterior fossa surgery
Classical TN with vascular compression visible on MRI
Age typically under 70 (though elderly patients with good fitness also benefit)
Failed medications (carbamazepine/oxcarbazepine) or intolerable side effects
Preference for long-term durable relief with preserved sensation
No previous major posterior fossa surgery
→ Percutaneous Procedures Preferred
Elderly patients or those with significant comorbidities making general anaesthesia high risk
Patients who decline open surgery
No compressing vessel identified on MRI (Glycerol/RF still effective)
TN due to multiple sclerosis (ablative procedures more appropriate)
Previous MVD with TN recurrence (re-operation possible but percutaneous simpler)
Patient accepts possibility of facial numbness as acceptable trade-off
What to Expect
Your MVD Patient Journey
at KG Hospital
From first consultation to return to normal life — here is what a typical MVD patient journey looks like at KG Hospital Coimbatore.
1
Neurosurgery Consultation & MRI Review
Your neurosurgeon reviews your history and your MRI. A high-quality MRI with dedicated trigeminal nerve protocol sequences (FIESTA/CISS) is required to visualise the compressing vessel. If your current MRI is inadequate, a repeat study is requested. Your neurosurgeon will explain treatment options and recommend the most appropriate approach.
Day 1 — OPD consultation, 45–60 minutes
2
Pre-operative Assessment
Blood tests, ECG, chest X-ray, and anaesthesia assessment. Any medical conditions (hypertension, diabetes, anticoagulants) are optimised. Anticoagulants and antiplatelet drugs are usually stopped 5–7 days before surgery. Admission to hospital the evening before or morning of surgery.
1–2 days before surgery
3
MVD Surgery
General anaesthesia. A small incision behind the ear, a 3–4 cm circular craniotomy in the posterior fossa. The TIVATO 700 microscope is used throughout. The trigeminal nerve root is identified. The compressing vessel is identified, gently mobilised, and a Teflon pad placed. The incision is closed. Most procedures take 2–3 hours.
2–3 hours in theatre
4
Post-operative Recovery
Recovery in Neuro ICU overnight. Common post-operative symptoms: mild headache (managed with analgesia), facial numbness in the surgical area (temporary), and occasionally some nausea. Most patients report their TN pain is gone on waking. Eating and drinking typically resumable the following day.
First 12–24 hours in Neuro ICU
5
Ward Recovery
Transfer to neurosurgery ward. Physiotherapy for mobilisation. Wound check. Discharge with oral analgesia, wound care instructions, and a follow-up appointment. Most patients are eating and mobile within 24–48 hours. Medications (carbamazepine) are gradually tapered over 4–6 weeks under neurology guidance.
Days 1–4 post-surgery
6
Discharge & Follow-up
Discharge day 3–5. Driving resumable at 4–6 weeks. Full return to work in 2–4 weeks depending on occupation. Follow-up at 2 weeks (wound check), 6 weeks, and 3 months. Carbamazepine is gradually reduced and stopped in the months following successful MVD — most patients no longer need medication.
Day 3–5 — discharge home